Understanding Bartholin’s Abscess: Causes, Symptoms, Treatment, and Prevention
A Bartholin’s abscess represents a painful medical condition affecting the female reproductive system. This condition develops when specialized glands near the vaginal opening become infected, leading to significant discomfort and requiring prompt medical attention. Understanding this condition helps individuals recognize symptoms early and seek appropriate treatment.
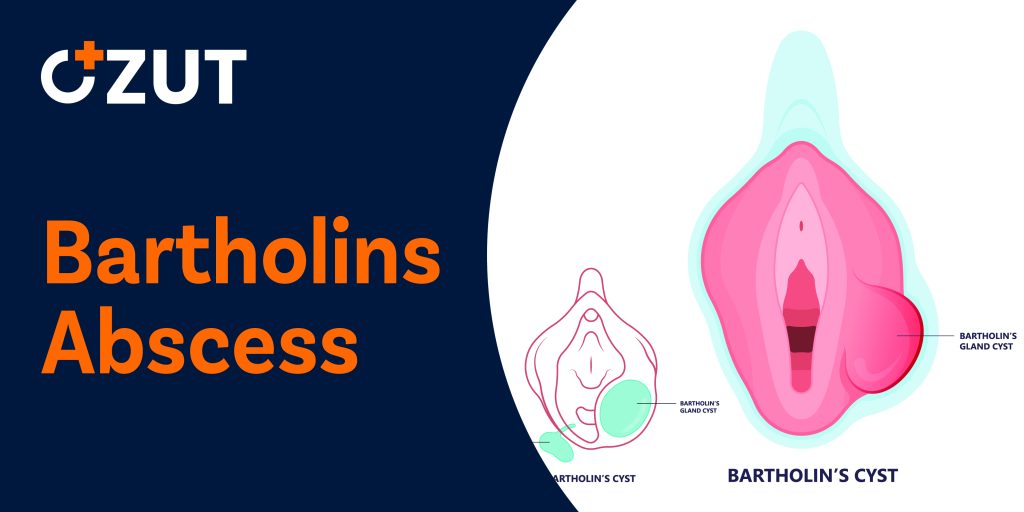
What Is a Bartholin’s Abscess
The condition occurs when one of two small glands positioned on either side of the vaginal opening develops an infection. These glands, each approximately the size of a pea, serve an important physiological function by providing natural lubrication to the vaginal area. When these glands become blocked, fluid accumulates and forms a cyst. If bacteria invade this cyst, infection develops and transforms it into an abscess.
The abscess can grow larger than one inch in diameter and typically causes substantial pain. The condition usually affects only one side at a time, though both glands remain susceptible to infection. While most individuals recover completely with proper treatment, some experience recurrent episodes requiring additional medical intervention.
Understanding the Anatomy and Function
The glands involved in this condition play a crucial role in maintaining vaginal health. Located at the entrance of the vaginal canal, these structures continuously produce secretions that keep the vaginal mucosa properly lubricated. This natural lubrication serves multiple purposes, including maintaining tissue health and facilitating comfortable physical activity.
Under normal circumstances, these glands function without notice. However, when blockages occur, the delicate balance of fluid production and drainage becomes disrupted. This disruption creates an environment where infection can take hold and develop into a more serious condition.
Causes and Risk Factors
Medical professionals have identified several bacterial sources that contribute to abscess formation. Common bacteria found in the digestive system can migrate to the vaginal area and cause infection. Additionally, sexually transmitted infections represent significant risk factors for developing this condition.
When harmful bacteria enter the gland, several processes occur simultaneously. Swelling begins as the body responds to the bacterial invasion. The gland opening may become obstructed, preventing normal drainage. As fluid continues to accumulate, pressure builds within the confined space. This process can take years to develop into a noticeable cyst, but once infection sets in, abscess formation can occur rapidly.
Bacterial Invasion Process
The progression from healthy gland to infected abscess follows a predictable pattern. Initially, bacteria colonize the gland opening or duct. The body’s immune response causes inflammation and swelling. As swelling increases, the narrow duct becomes blocked, trapping fluid inside. Bacteria multiply in this enclosed environment, producing pus and increasing pressure. Eventually, the infection reaches a critical point where the abscess may rupture through the skin.
Recognizing Symptoms and Signs
Identifying this condition early improves treatment outcomes significantly. The most noticeable symptom involves the formation of a lump beneath the skin on one side of the vaginal opening. This lump may start small but can grow rapidly as infection progresses.
Pain represents the primary complaint among those affected. This discomfort intensifies during activities that apply pressure to the affected area. Walking becomes uncomfortable as the legs move and create friction. Sitting down puts direct pressure on the abscess, causing sharp or throbbing pain. Sexual activity becomes particularly painful and may be impossible during active infection.
Progressive Symptom Development
As the condition advances, additional symptoms may emerge. The affected area often becomes red and warm to the touch, indicating active inflammation. Swelling may extend beyond the immediate abscess site. Some individuals develop fever as the body fights the infection. The abscess may begin draining spontaneously, producing discharge that can be clear, bloody, or contain pus.
Diagnostic Procedures
Proper diagnosis requires professional medical evaluation. Healthcare providers conduct thorough physical examinations to assess the affected area. During examination, the provider checks for characteristic lumps and evaluates the extent of swelling and inflammation. The size, location, and tenderness of any masses provide important diagnostic information.
Laboratory testing may be necessary to identify the specific bacteria causing infection. Samples collected from the affected area undergo analysis to detect sexually transmitted infections. This testing proves crucial because certain infections require specific antibiotic treatment. Identifying the causative organism allows providers to prescribe the most effective medication.
Home Treatment Approaches
Early-stage management sometimes succeeds with conservative home treatments. Warm water soaking provides the foundation for initial care. This approach involves sitting in shallow, warm water for extended periods multiple times daily. The warmth promotes blood flow to the affected area and may encourage natural drainage.
Treatment protocols typically recommend soaking sessions lasting ten to fifteen minutes. These sessions should occur three to four times throughout the day. Consistency matters significantly, as single sessions rarely produce meaningful results. The process may require many days of dedicated treatment before improvement becomes noticeable.
Natural Remedies and Supportive Care
Some individuals explore additional home remedies to complement warm water therapy. Certain plant-based oils possess properties that may support healing. Tea tree oil demonstrates antibacterial characteristics that could help combat infection. Castor oil may improve blood circulation in the affected region, potentially reducing inflammation. When combined and applied topically, these oils might promote drainage and healing.
However, home treatments have significant limitations. The gland opening remains extremely small, making complete drainage difficult without medical intervention. The opening may close prematurely, trapping infection inside and allowing the condition to worsen. Therefore, home care should never replace professional medical evaluation and treatment.
Medical Treatment Options
Professional medical intervention typically becomes necessary for complete resolution. Surgical drainage represents the standard treatment approach. This procedure can often be performed in an outpatient setting using local anesthesia to numb the area. Some situations may warrant general anesthesia in a hospital environment, particularly for anxious patients or complex cases.
During the drainage procedure, the healthcare provider makes a small incision in the abscess. This opening allows accumulated pus and fluid to escape. A small tube called a catheter is then inserted into the cavity. This catheter remains in place for several weeks, ensuring continuous drainage and preventing premature closure. Once healing progresses sufficiently, the catheter is either removed by the provider or allowed to fall out naturally.
Antibiotic Therapy
Medication plays an important role in treating the underlying infection. Antibiotics target the bacteria causing the abscess, helping the body eliminate the infection more effectively. However, antibiotic necessity depends on individual circumstances. If drainage proves adequate and infection markers decrease, antibiotics may not be required. Healthcare providers make this determination based on examination findings and laboratory results.
Advanced Surgical Interventions
Recurrent cases require more aggressive treatment strategies. When abscesses return repeatedly despite standard drainage procedures, a specialized surgery called marsupialization may be recommended. This procedure differs from simple drainage in an important way.
During marsupialization, the surgeon creates an opening in the abscess and then stitches the edges of this opening to surrounding tissue. This technique creates a permanent drainage pathway, significantly reducing recurrence risk. The opening remains patent, allowing any future fluid accumulation to drain freely rather than forming another abscess.
The procedure can be performed under local or general anesthesia depending on patient preference and clinical factors. A catheter may be placed temporarily, or special gauze packing might be used overnight. Any active infection receives antibiotic treatment before surgery to optimize outcomes.
Gland Removal Surgery
In rare cases where all other treatments fail, complete gland removal becomes necessary. This surgery represents the most definitive treatment but is reserved for severe, recurrent cases. The procedure requires general anesthesia and hospital admission. Recovery takes longer than other treatment options, but recurrence becomes impossible once the glands are removed.
Prevention Strategies
While no method guarantees complete prevention, certain practices reduce infection risk significantly. Safe sexual practices form the foundation of prevention efforts. Using barrier protection during intimate contact prevents transmission of bacteria and sexually transmitted infections. Regular testing for sexually transmitted infections allows early detection and treatment before complications develop.
Maintaining excellent hygiene in the genital area helps keep harmful bacteria away. Gentle cleansing with mild soap and water proves sufficient for most individuals. Avoiding harsh chemicals or douching preserves the natural bacterial balance that protects against infection.
Urinary Tract Health
Supporting urinary tract health may indirectly reduce abscess risk. Drinking adequate fluids throughout the day helps flush bacteria from the urinary system. Avoiding prolonged delays in urination prevents bacterial multiplication. Some individuals benefit from cranberry supplements, which may support urinary tract health through various mechanisms.
Potential Complications
Untreated abscesses can lead to serious health consequences. As infection progresses, bacteria may spread beyond the initial site. Surrounding tissues can become involved, expanding the infected area. In severe cases, bacteria enter the bloodstream, creating a dangerous condition called septicemia.
Bloodstream infections represent medical emergencies requiring immediate hospitalization. Bacteria circulating throughout the body can affect multiple organ systems simultaneously. This widespread infection can become life-threatening without prompt, aggressive treatment.
Warning Signs Requiring Immediate Care
Certain symptoms indicate serious complications requiring urgent medical attention. Fever exceeding one hundred three degrees Fahrenheit suggests severe infection. Sudden abscess rupture, while sometimes relieving pressure, can spread infection. Pain that fails to improve or worsens despite treatment warrants immediate evaluation. Any signs of systemic illness, including confusion, rapid heartbeat, or difficulty breathing, require emergency care.
When to Seek Medical Attention
Professional evaluation should occur whenever abscess symptoms develop. Early medical intervention prevents complications and speeds recovery. Individuals experiencing fever alongside abscess symptoms need prompt assessment. Pain interfering with normal daily activities justifies immediate medical consultation.
Delaying treatment allows infection to progress and increases complication risk. Healthcare providers can assess severity, provide appropriate treatment, and monitor for potential complications. Even if symptoms seem mild initially, professional evaluation ensures proper diagnosis and management.
Recovery and Prognosis
Most individuals experience rapid improvement following proper treatment. After successful drainage, many people feel significantly better within twenty-four hours. Pain decreases markedly, and swelling begins to subside. Normal activities can usually resume gradually as healing progresses.
Surgical treatment requires longer recovery periods. The first few days after surgery should involve maximum rest. Following provider instructions carefully ensures optimal healing. Any prescribed antibiotics must be completed as directed, even if symptoms improve quickly. Incisions need time to heal completely before resuming all normal activities.
Long-Term Outlook
Successfully treated abscesses typically leave no lasting effects beyond possible minor scarring. The scarring usually remains minimal and causes no functional problems. Most individuals return to completely normal function once healing completes. However, some people experience recurrent episodes requiring ongoing monitoring and potentially more aggressive treatment approaches.
Living With Recurrent Cases
Some individuals face repeated abscess formation despite appropriate treatment. These recurrent cases require ongoing medical management and may necessitate advanced surgical interventions. Working closely with healthcare providers helps develop effective long-term management strategies. Understanding triggers and early warning signs allows prompt intervention when symptoms recur.
Maintaining open communication with healthcare providers proves essential for managing recurrent cases. Regular follow-up appointments allow monitoring for early recurrence signs. Discussing concerns and treatment preferences helps ensure care aligns with individual needs and circumstances.