Understanding Prostate Enlargement: Comprehensive Guide to Symptoms, Diagnosis, and Treatment Options
Prostate enlargement represents a common condition affecting aging men, characterized by the expansion of the prostate gland and surrounding tissue. This natural biological process occurs in two distinct phases throughout a man’s lifetime. The initial growth phase happens during early puberty when the prostate doubles in size. The second phase begins around age twenty-five and continues throughout most of adult life. As men advance in years, the prostate may continue enlarging, potentially reaching a size that creates significant health challenges.
When the prostate enlarges substantially, it exerts pressure against the urethra, the tube responsible for carrying urine from the bladder through the penis. This compression triggers a cascade of physiological changes. The bladder wall gradually thickens in response to increased resistance, and over time, the bladder may weaken and lose its capacity to empty completely. Residual urine remaining in the bladder after urination creates numerous lower urinary tract complications. Understanding how prostate enlargement causes these symptoms helps healthcare providers determine appropriate treatment strategies tailored to individual patient needs.
The Prostate’s Role in Male Reproductive Health
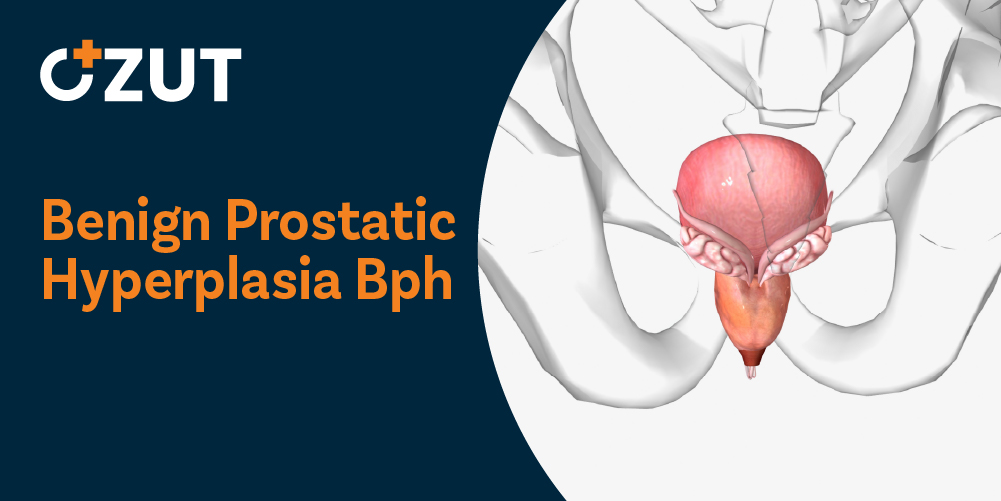
The prostate serves as an essential component of the male reproductive system, with its primary function being the production of fluid that forms part of semen. This walnut-sized gland typically weighs approximately one ounce and occupies a strategic position below the bladder and anterior to the rectum. The prostate encircles the urethra, making its size and condition directly relevant to urinary function. When functioning normally, the prostate maintains a size that allows unobstructed urine flow, but enlargement can significantly compromise this delicate balance.
Identifying Risk Factors for Prostate Enlargement
Several demographic and lifestyle factors increase the likelihood of developing prostate enlargement. Age stands as the most significant risk factor, with men over fifty experiencing substantially elevated risk as they continue aging. Genetic predisposition plays an important role, as men whose fathers experienced prostate enlargement face higher probability of developing the condition themselves. Body weight significantly influences risk, with overweight and obese men showing increased susceptibility. Physical inactivity contributes to higher risk levels, while some men experiencing erectile dysfunction may also face elevated chances of prostate enlargement.
Recognizing Common Symptoms and Warning Signs
When the prostate enlarges sufficiently to affect bladder function, it can irritate or obstruct normal urinary processes. Frequent urination emerges as one of the most prevalent symptoms, with affected men often needing to urinate every one to two hours, particularly during nighttime hours. This symptom alone can significantly impact quality of life and sleep patterns.
Comprehensive Symptom Profile
Incomplete emptying represents a frustrating symptom where men feel their bladder remains full even immediately after urination. Frequency manifests as the persistent need to urinate approximately every one to two hours throughout the day and night. Intermittency describes the need to stop and restart multiple times during a single urination attempt, creating prolonged bathroom visits. Urgency involves sudden, intense needs to urinate with minimal warning, sometimes making it difficult to reach facilities in time.
Weak stream characterizes reduced urine flow force, often described as a trickle rather than a steady stream. Straining encompasses difficulty initiating urination or the need to push forcefully to begin or maintain urine flow. Nocturia specifically refers to waking two or more times nightly to urinate, severely disrupting sleep quality and contributing to daytime fatigue. These symptoms collectively impact daily activities, social interactions, and overall wellbeing, making proper diagnosis and treatment essential for maintaining quality of life.
Understanding the Underlying Causes
The precise causes of prostate enlargement remain incompletely understood, though the condition predominantly affects older men, suggesting age-related factors play crucial roles. Hormonal changes appear central to the development process, with testosterone from the testes potentially serving as the primary contributing factor. As men age, active testosterone levels in the bloodstream decline while the company levels remain relatively stable. This shifting hormonal balance may trigger prostate cell growth and proliferation.
Another significant theory focuses on dihydrotestosterone, a male hormone essential for prostate development. Research indicates that older men often maintain elevated levels of this hormone even as testosterone levels decrease. This hormonal imbalance may stimulate continued prostate growth beyond normal parameters, leading to the enlargement that causes urinary symptoms. The interplay between these various hormones creates a complex biological environment that researchers continue studying to develop more effective treatments.
Diagnostic Testing and Evaluation Methods
Symptom Assessment Tools
Healthcare providers utilize standardized symptom scoring systems to evaluate urinary changes and their severity. These assessment tools help classify prostate enlargement from mild to severe categories. Patients rate various urinary symptoms, providing healthcare providers with quantifiable data to guide treatment decisions. This initial diagnostic step, combined with comprehensive medical history review, establishes baseline information essential for monitoring condition progression and treatment effectiveness.
Physical Examination Procedures
Digital rectal examination remains a fundamental diagnostic tool despite its brief duration of ten to fifteen seconds. During this examination, patients either lie on their side or bend forward while the healthcare provider inserts a gloved, lubricated finger into the rectum. This allows direct palpation of the prostate’s posterior wall, enabling detection of enlargement, tenderness, lumps, or abnormal firm areas. This simple yet informative examination provides crucial information about prostate size, texture, and potential abnormalities requiring further investigation.
Urine Testing Protocols
Multiple urine tests assess bladder function and urethral patency. Urinalysis examines urine samples for blood, the company indicators, glucose, protein, and other factors that help identify symptom causes. These tests also screen for bladder malignancies, making them important for comprehensive urinary health assessment. Immediate medical attention becomes necessary when urine contains blood, urination causes pain or burning sensations, or complete urinary retention occurs.
Post-void residual volume measurement quantifies urine remaining in the bladder after urination, providing direct evidence of incomplete emptying. Uroflowmetry measures urine flow rate, offering objective data about urethral obstruction severity. Urodynamic pressure flow studies assess bladder pressure during urination, revealing how effectively the bladder contracts and whether obstruction impedes normal function. These measurements collectively provide comprehensive information about lower urinary tract function.
Advanced Imaging Techniques
Imaging studies visualize prostate size, shape, and anatomical relationships with surrounding structures. Ultrasound examinations use sound waves to create internal images showing prostate dimensions and characteristics. Cystoscopy involves inserting a specialized scope through the urethra to directly visualize the urinary passage and bladder interior. When surgical intervention becomes necessary, magnetic resonance imaging and computed tomography provide exceptionally detailed anatomical information. These advanced scans precisely map prostate enlargement patterns and surrounding tissue relationships, enabling surgical planning and approach optimization.
Blood Testing for Cancer Screening
When malignancy concerns arise, blood tests measure prostate-specific antigen levels. This protein, produced exclusively by prostate tissue, normally appears in minimal blood concentrations. Rapid increases may indicate various conditions including enlargement, inflammation, or cancer. Patients should avoid sexual activity several days before testing, as this can artificially elevate readings. While elevated levels warrant investigation, they do not definitively indicate cancer, as non-cancerous conditions also raise these measurements.
Treatment Options and Management Strategies
Active Surveillance Approach
Many cases require only careful monitoring without active intervention. This approach involves regular follow-up visits, typically annually, where healthcare providers assess symptom progression and emerging complications. Active surveillance suits men with mild to moderate symptoms who remain unbothered by their condition’s effects. Diet optimization and regular exercise often help prevent symptom worsening and may improve existing complaints. This conservative strategy avoids treatment risks while maintaining close observation for changes requiring intervention.
Pharmaceutical Interventions
Several medication classes effectively manage prostate enlargement symptoms. Alpha blockers relax prostate and bladder muscles, improving urine flow when obstruction exists. These medications begin working immediately, though they do not reduce prostate size. Side effects may include dizziness, lightheadedness, fatigue, and ejaculation difficulties. Men with moderate to severe symptoms who find them bothersome represent ideal candidates, though those planning cataract surgery should discuss timing with their healthcare providers.
Five-alpha reductase inhibitors increase urine flow and reduce prostate size by blocking dihydrotestosterone production. This male hormone accumulates in prostate tissue and stimulates growth. These medications may reduce complication risks and surgical necessity, though they require months to achieve full effectiveness. Side effects include erectile dysfunction and decreased libido. Continuous use prevents symptom recurrence, making these medications particularly suitable for men with substantially enlarged prostates.
Combined therapy utilizes both medication classes simultaneously, often producing superior results compared to either drug alone. This approach may prevent condition progression more effectively, though it increases side effect risks. Potential adverse effects include dizziness, erectile dysfunction, weakness, fatigue, and orthostatic hypotension. Healthcare providers may add antimuscarinic medications for patients experiencing overactive bladder symptoms characterized by uncontrollable bladder muscle contractions causing urgent, frequent urination and potential incontinence. Men with larger prostates typically benefit most from combination approaches.
Minimally Invasive Surgical Procedures
Less invasive surgical techniques often proceed as outpatient procedures without hospital admission, offering quicker recovery compared to traditional surgery. These approaches provide symptom relief including improved urinary control, though some procedures carry higher retreatment rates. Patients should discuss long-term effectiveness and potential need for additional interventions when considering these options.
Prostatic urethral lift employs tiny implants placed through needles into prostate tissue. These permanent implants lift and compress enlarged tissue away from the urethra, restoring normal urine flow. The procedure uses local or general anesthesia without external incisions, and tissue remains intact rather than being destroyed or removed. This approach produces fewer sexual side effects compared to other surgical options. Patients should discuss potential impacts on future imaging studies and any metal allergies before proceeding. Current research demonstrates effectiveness for at least five years.
Water vapor thermal therapy uses steam to destroy prostate cells compressing the urethra. This office-based procedure uses local anesthesia or oral pain medication. A specialized handheld device with a needle tip combines radiofrequency energy and water to generate steam, causing rapid cell death. Natural healing processes remove dead tissue, reducing prostate size. Candidates include men preferring to avoid medication, those for whom drugs proved ineffective, and men seeking to minimize sexual side effects. Temporary blood in urine and catheter use may occur, with painful or frequent urination typically resolving within two to three weeks.
Temporary implanted devices remain in the prostatic urethra for approximately one week before removal. These devices reshape the urinary channel, modestly reducing obstruction and improving symptoms. This low-risk procedure can occur in operating rooms or office settings. Potential side effects include urinary tract infections, incontinence, urethral scarring, and temporary urinary urgency or burning sensations.
the company blocks blood flow to the prostate, attempting to shrink the entire gland. This radiologic procedure shows short-term symptom improvement, though long-term effectiveness data remains limited. Current evidence suggests benefits lasting less than one year, with insufficient data to recommend this approach over more established therapies for routine treatment.
Catheterization uses tubes to drain urine from the bladder, either through the urethra or via small punctures above the pubic bone. This option helps men with bladder control problems and prostatic obstruction, though benefits remain temporary and the company risks exist. Clean intermittent catheterization involves placement and removal every six to eight hours by patients or caregivers. Indwelling catheters remain in place for extended periods. This approach suits men awaiting medication effectiveness, preparing for surgery, managing infections, or near end of life when surgery is inadvisable.