Understanding Testicular and Epididymal Inflammation: Comprehensive Guide to Symptoms, Causes, and Treatment Options
Discomfort in the scrotal region represents a common medical concern affecting males across various age groups. This condition typically involves inflammation of the reproductive structures, specifically the coiled tube that stores developing reproductive cells and the reproductive glands themselves. Understanding these conditions, their underlying causes, and available treatment options is essential for proper management and recovery.
Defining the Conditions: Types of Scrotal Inflammation
Inflammation in the scrotal area can manifest in several distinct forms, each with unique characteristics and progression patterns. The primary conditions include inflammation of the storage tube, inflammation of the reproductive gland, or combined inflammation affecting both structures simultaneously.
Inflammation of the Coiled Storage Tube
This condition occurs when the coiled tube behind the reproductive gland becomes inflamed. The condition can present in two distinct forms: acute and chronic. The acute form develops rapidly with pronounced symptoms including redness and pain, typically responding well to appropriate medical intervention. Symptoms appear suddenly and resolve with proper treatment within a reasonable timeframe.
The chronic form presents differently, characterized by a duller, persistent discomfort that develops gradually over time. This long-term condition often proves more challenging to manage, as symptoms may improve with treatment but rarely disappear completely. Patients frequently experience intermittent flare-ups, with symptoms recurring periodically even after initial improvement. This condition predominantly affects adult males.
Inflammation of the Reproductive Gland
Isolated inflammation of the reproductive gland occurs less frequently than inflammation of the storage tube. This condition almost exclusively presents in acute form, developing rapidly with sudden onset of symptoms. With appropriate treatment, the acute inflammation typically resolves completely. The chronic form remains poorly understood and is generally considered part of a broader condition involving persistent discomfort in the scrotal region.
Combined Inflammatory Condition
When both the storage tube and the reproductive gland become inflamed simultaneously, the condition represents a more complex presentation. This combined inflammation typically develops suddenly and requires comprehensive treatment addressing both affected structures.
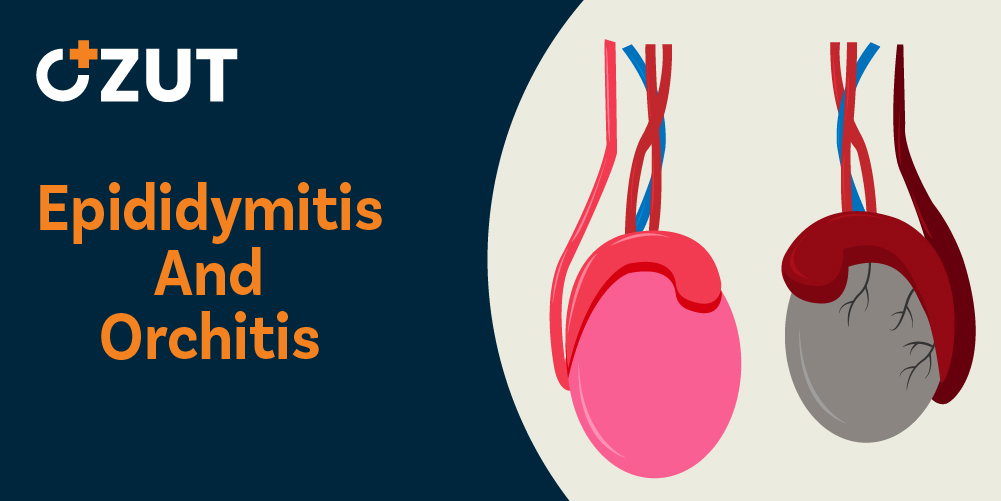
Normal Anatomy and Function of Male Reproductive Structures
The male reproductive system performs three critical functions: production, storage, and transport of reproductive cells. These cells develop through specialized hormonal processes within two glands located in the scrotal sac at the base of the reproductive organ.
Reproductive cells begin their development within the glands and continue maturing as they move through the coiled storage tube located behind each gland. This tube connects to the ejaculatory passage through a transport tube that runs from the lower scrotum into the inguinal canal, then through the pelvic region behind the bladder.
At the junction where the transport tube meets the seminal storage structure, the ejaculatory passage forms. During ejaculation, fluid from the seminal storage structures and the accessory gland combines with reproductive cells to form the ejaculate, which travels through the urethral passage and exits through the reproductive organ.
Recognizing Symptoms: Acute Presentations
The primary symptom patients notice is discomfort in the scrotal region. Pain typically begins at the posterior aspect of one reproductive gland but can rapidly spread throughout the entire gland, scrotum, and sometimes extend into the groin area.
Physical Manifestations
The scrotal skin may exhibit several visible changes during acute inflammation:
- Swelling and enlargement of affected tissues
- Tenderness upon touch or movement
- Redness and color changes in the skin
- Firmness and increased tissue density
- Warmth radiating from the affected area
- Fluid accumulation causing scrotal swelling
Associated Infection Symptoms
Scrotal infections may originate from infections elsewhere in the body, producing symptoms both locally and in other regions. Different infection sources produce characteristic symptom patterns.
Urethral infections cause pain and burning during urination, possible blood in urine, and discomfort in the reproductive organ and groin. Bladder infections produce lower abdominal pain, frequent urgent urination with burning sensations. Accessory gland infections create discomfort between the scrotum and anus, along with frequent urgent urination and burning. Kidney infections manifest with fever and flank pain.
Chronic Condition Characteristics
Chronic inflammation presents distinctly from acute conditions. Pain remains localized within the scrotum without spreading to surrounding areas. The intensity is notably less severe than acute presentations, and symptoms may fluctuate, sometimes requiring medication and other times resolving independently. Unlike acute conditions, the scrotal skin does not display swelling, tenderness, redness, firmness, or warmth.
Viral-Related Inflammation Symptoms
When viral infections cause reproductive gland inflammation, symptoms can be uncommon and distinctive. Pain may begin in one gland and spread throughout the scrotum. Physical changes include swelling, tenderness, redness, firmness, and warmth of the scrotal skin. Patients may develop fever, and the entire scrotum can become swollen and painful.
Viral inflammation caused by the mumps virus produces specific symptoms including mild to severe pain, marked tenderness, and significant swelling. When mumps is the underlying cause, testicular pain may appear up to seven days after facial gland swelling occurs.
Understanding the Causes: Acute Bacterial Infections
Acute inflammation most commonly results from bacterial infections. Common intestinal bacteria frequently cause these infections through various pathways depending on patient age and circumstances.
Age-Specific Causes
In prepubescent children, infections typically originate in the bladder or kidney before spreading to the reproductive structures. Some boys require additional testing to identify underlying urinary tract abnormalities predisposing them to infections.
In sexually active men, particularly those under forty, sexually transmitted infections represent a primary cause. These infections commonly involve specific bacteria that initially infect the urethra before ascending to the reproductive structures. Urethral discharge may accompany these infections.
Additional Causative Factors
Several other conditions can trigger inflammation:
- Enlarged accessory gland obstructing bladder outflow
- Bacterial infection of the accessory gland
- Partial urethral obstruction
- Recent catheter insertion or use
Less Common Causes
Uncommon causes include urine flowing backward into the storage tube, creating the company or inflammatory non-bacterial inflammation. This often occurs after heavy lifting when urine causes swelling without actual infection. Certain cardiac medications rarely cause inflammation. Bloodstream infections, such as tuberculosis, can also spread to reproductive structures.
Chronic Inflammation Origins
Chronic inflammation may develop following acute episodes that fail to resolve completely. Alternatively, it can develop without preceding acute symptoms or identifiable infection. In such cases, the underlying cause often remains unknown, making treatment more challenging.
Viral Causes and Isolated Gland Inflammation
Isolated reproductive gland inflammation predominantly results from viral infections, particularly mumps. Approximately one-third of males who contract mumps after puberty develop reproductive gland inflammation. This complication only occurs in post-pubertal males. In some cases, antiviral medication can prevent gland inflammation when administered during mumps infection. Viral inflammation typically does not spread to the storage tube.
Combined Inflammation Causes
Combined inflammation affecting both the storage tube and reproductive gland most commonly results from bacterial infections. Rarely, tuberculous infections can cause this combined presentation, though such cases are uncommon in developed countries.
Diagnostic Approaches and Testing Methods
Healthcare providers employ multiple diagnostic strategies to identify the specific condition and underlying cause. The evaluation begins with comprehensive medical history review and physical examination. Providers assess symptom onset, duration, severity, and associated symptoms.
Laboratory Testing
Urine sample analysis represents a fundamental diagnostic tool. Providers examine urine microscopically to identify bacteria and may culture the sample to identify specific organisms. In acute storage tube inflammation, urine commonly shows infection. In chronic cases, urine typically appears uninfected.
When urethral infection is suspected, providers may collect urethral fluid samples using swabs to test for sexually transmitted infections or bacterial presence. This testing helps guide appropriate antibiotic selection.
Imaging Studies
For patients experiencing sudden severe pain, ultrasound imaging provides detailed visualization of scrotal structures. This non-invasive test uses sound waves to create images, measuring blood flow in the storage tube, examining internal gland structure, and identifying other abnormalities in the region.
Treatment Strategies: Acute Conditions
Treatment for acute inflammation typically begins with antibiotic therapy lasting one to two weeks. Most patients can take oral medications as outpatients. Antibiotic selection depends on the identified bacterial organism.
Common Antibiotic Options
Frequently prescribed antibiotics include medications from the tetracycline family, fluoroquinolone class, and combination sulfa drugs. The specific choice depends on suspected or confirmed bacterial type, patient allergies, and local resistance patterns.
Hospitalization Criteria
Severe infections may require hospital admission for intravenous antibiotic administration. Hospitalization becomes necessary when patients experience uncontrollable pain, persistent vomiting, high fever, or fail to improve with oral antibiotics. Occasionally, narcotic pain medications are needed for a few days in severe cases.
Specialized Treatment Scenarios
Tuberculous inflammation, though rare, requires specialized anti-tuberculous medications. Severe cases with extensive damage may necessitate surgical removal of affected structures. Medication-induced inflammation is managed by reducing or discontinuing the causative drug under medical supervision. Non-infectious inflammation lacks standardized treatment protocols.
Supportive Care Measures
Regardless of underlying cause, supportive care plays a crucial role in recovery. Rest for one to two days with scrotal elevation above heart level improves blood flow, reduces swelling and pain, and promotes healing. Intermittent ice application provides additional symptom relief. Adequate fluid intake supports recovery in infectious cases.
Anti-inflammatory medications like common over-the-counter pain relievers reduce both pain and the swelling causing discomfort. Severe pain may warrant short-term narcotic medication, though this is minimized whenever possible.
Managing Chronic Conditions
Chronic inflammation management focuses on symptom control through medications and comfort measures. Pain medication and heat application represent standard treatments. When symptoms persist despite conservative management, providers may recommend alternative pain medications or referral to pain management specialists.
If all conservative measures fail, surgical removal of the storage tube may be considered while preserving the reproductive gland. This option is reserved for refractory cases significantly impacting quality of life.
Treating Isolated Gland Inflammation
Bacterial gland inflammation responds well to appropriate antibiotics. Pain medication helps manage symptoms during treatment. Viral inflammation, particularly mumps-related cases, lacks specific treatment and typically resolves spontaneously over time with supportive care.
Recovery Timeline and Expectations
For infectious acute conditions, patients typically begin feeling better within two to three days of starting antibiotics. Failure to improve or persistent redness warrants prompt medical follow-up. Some discomfort may persist for weeks to months after completing antibiotic courses. Swelling resolution may take several months. Rest with scrotal elevation for one to two days accelerates