Understanding the Menstrual Cycle: A Complete Guide to Reproductive Health
The menstrual cycle represents one of the most fundamental aspects of female reproductive health, yet many individuals lack comprehensive understanding of this natural biological process. This guide provides detailed information about cycle length, hormonal changes, ovulation, and fertility to help individuals better understand their bodies and reproductive health.
Menstrual Cycle Length and Variation
The menstrual cycle encompasses the time from the first day of one period to the day before the next period begins. While individual variation is common and completely normal, the average cycle length is approximately 28 days. However, regular cycles ranging from 21 to 35 days fall within normal parameters and should not cause concern.
The menstrual cycle begins counting from day one, which is marked by the first day of menstrual bleeding. Understanding this counting method is essential for tracking fertility, planning or preventing pregnancy, and monitoring overall reproductive health. Women who track their cycles often notice patterns that help them predict when their next period will arrive.
Age-Related Milestones in Menstruation
The onset of menstruation, known as menarche, typically occurs around age 12, though girls can begin menstruating anywhere from age 8 onwards. This wide range reflects normal variation in physical development and should not be considered abnormal unless accompanied by other concerning symptoms.
At the other end of the reproductive lifespan, menopause typically occurs around age 51. This marks the cessation of menstrual periods and the end of natural fertility. Between these two milestones, spanning approximately 40 years from age 12 to 52, most individuals will experience around 480 menstrual cycles, though this number decreases with each pregnancy.
The Reproductive Anatomy
To fully comprehend the menstrual cycle, understanding the female reproductive anatomy is essential. The reproductive system consists of several interconnected organs, each playing a crucial role in the monthly cycle and potential pregnancy.
Key Reproductive Organs
The reproductive system includes five primary components that work together throughout the menstrual cycle:
- Two ovaries that store, develop, and release eggs throughout the reproductive years
- The uterus, commonly called the womb, where a fertilized egg implants and develops into a baby
- Two fallopian tubes, thin passages connecting the ovaries to the uterus
- The cervix, which serves as the entrance to the uterus from the vaginal canal
- The vagina, the muscular canal connecting the external genitalia to the cervix
Each of these organs responds to hormonal signals throughout the menstrual cycle, preparing the body for potential pregnancy each month. When pregnancy does not occur, the cycle resets and begins again.
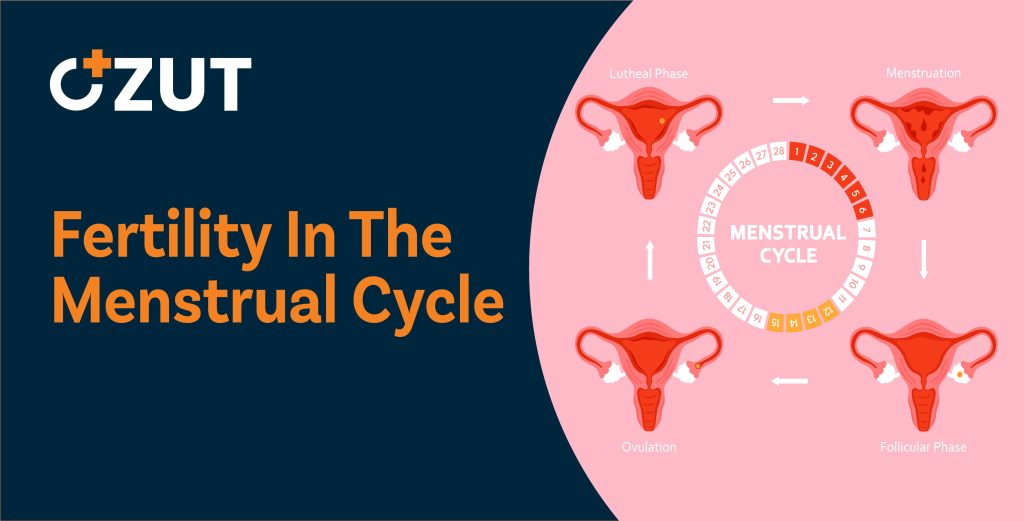
Hormonal Control of the Menstrual Cycle
The menstrual cycle operates under precise hormonal control, with two primary hormones orchestrating the monthly changes: estrogen and progesterone. These hormones rise and fall in predictable patterns, triggering specific events throughout the cycle.
The Role of Estrogen
During the first half of the menstrual cycle, estrogen levels gradually increase. This rising estrogen triggers two important events: it causes an egg within the ovary to mature and develop, and it stimulates the uterine lining to thicken in preparation for potential pregnancy. The peak in estrogen levels ultimately triggers ovulation, the release of the mature egg from the ovary.
Progesterone and the Second Half
After ovulation occurs, progesterone becomes the dominant hormone. Progesterone further prepares the uterine lining for implantation of a developing embryo. It creates an optimal environment for pregnancy by making the uterine lining receptive to a fertilized egg and maintaining this environment should pregnancy occur.
When pregnancy does not occur, both estrogen and progesterone levels drop sharply. This hormonal decline triggers the breakdown of the uterine lining, which is then shed from the body as menstrual flow. This shedding marks the beginning of a new cycle.
Understanding Menstruation
Menstruation, commonly called a period, consists of blood and uterine lining tissue that exits the body through the vagina. The first day of menstrual bleeding is designated as day one of the menstrual cycle, providing a clear starting point for cycle tracking.
Duration and Blood Loss
Typical menstrual periods last between 2 and 7 days, though this can vary among individuals and even from cycle to cycle for the same person. During a normal period, individuals lose approximately 20 to 90 milliliters of blood, equivalent to about 1 to 5 tablespoons.
Some individuals experience heavier bleeding than this average range. Heavy menstrual bleeding can impact quality of life and may indicate underlying health conditions. Medical interventions and treatments are available for those experiencing problematic heavy periods, and seeking medical advice is recommended when bleeding seems excessive.
The Process of Ovulation
Ovulation represents a critical event in the menstrual cycle and is essential for natural conception. During ovulation, a mature egg is released from one of the ovaries and begins its journey through the fallopian tube toward the uterus.
Egg Development and Release
Individuals are born with their complete lifetime supply of eggs. Once menstruation begins, typically one egg matures and is released during each menstrual cycle. This egg remains viable for fertilization for approximately 12 to 24 hours after its release.
The timing of ovulation typically occurs 10 to 16 days before the start of the next menstrual period. For individuals with regular 28-day cycles, ovulation commonly occurs around day 14. However, this timing varies significantly for those with shorter or longer cycles.
Multiple Egg Release
Occasionally, more than one egg may be released during a single ovulation event. If multiple eggs are fertilized by separate sperm, this can result in fraternal twins or other multiple pregnancies. This natural occurrence explains why some twins are not identical.
Fertility and Conception
Understanding fertility windows is crucial for both those trying to conceive and those seeking to prevent pregnancy. The fertile window represents the days during which sexual intercourse can result in pregnancy.
The Fertile Window
Theoretically, the fertile window is relatively short, centered around the time of ovulation. However, sperm can survive in the fallopian tubes for up to seven days after intercourse. This extended sperm survival means that intercourse occurring several days before ovulation can still result in pregnancy.
For individuals with regular 28-day cycles, the most fertile period typically occurs around day 14. However, this timing shifts for those with shorter or longer cycles. It is possible, though less likely, to become pregnant shortly after menstruation ends if ovulation occurs early or if the cycle is particularly short.
Pregnancy Without Penetration
While less common, pregnancy can occur even without full penetration. If sperm comes into contact with the vaginal area, there is a small risk of pregnancy. This can happen if ejaculation occurs very close to the vaginal opening or if an erect penis contacts the vulva or vaginal area. While the risk is low, it is not zero, and individuals should be aware of this possibility.
Hormonal Contraception and Ovulation
Many forms of hormonal contraception work by preventing ovulation altogether. Without ovulation, pregnancy cannot occur naturally. Common methods that prevent ovulation include combined oral contraceptives, contraceptive patches, and contraceptive injections.
These methods deliver synthetic hormones that suppress the natural hormonal fluctuations required for egg development and release. By maintaining steady hormone levels, these contraceptives prevent the hormonal surge that triggers ovulation, effectively preventing pregnancy.
Vaginal Secretions Throughout the Cycle
Vaginal secretions, sometimes called vaginal discharge, change in consistency and appearance throughout the menstrual cycle in response to hormonal fluctuations. These changes are normal and can actually help individuals identify their fertile window.
Ovulation-Related Changes
Around the time of ovulation, vaginal secretions typically become thinner, clearer, and more stretchy. The consistency often resembles raw egg white and can be stretched between fingers. This change in cervical mucus facilitates sperm transport and survival, supporting the possibility of conception during the fertile window.
After ovulation, as progesterone levels rise, vaginal secretions typically become thicker and less abundant. These cyclical changes are completely normal. However, unusual changes in color, odor, or consistency may indicate infection or other health issues and warrant medical evaluation.
Tracking Your Menstrual Cycle
Tracking the menstrual cycle provides valuable information about reproductive health and can help identify irregularities that may require medical attention. Many individuals use calendar methods, smartphone applications, or written journals to record cycle length, symptoms, and patterns.
Benefits of Cycle Tracking
Regular cycle tracking offers several advantages. It helps predict when the next period will arrive, identifies the fertile window for those trying to conceive or avoid pregnancy, and establishes baseline patterns that make irregularities more noticeable. Changes in cycle length, flow, or associated symptoms can provide early warning signs of health issues.
For those experiencing irregular cycles, tracking provides valuable information to share with healthcare providers. Detailed records of cycle length, bleeding patterns, and symptoms help medical professionals diagnose and treat menstrual disorders more effectively.
When to Seek Medical Advice
While variation in menstrual cycles is normal, certain symptoms warrant medical evaluation. Individuals should consult healthcare providers if they experience significant changes in cycle length, unusually heavy bleeding, severe pain, or bleeding between periods.
Signs Requiring Medical Attention
Several symptoms indicate the need for medical evaluation:
- Periods lasting longer than seven days consistently
- Bleeding requiring pad or tampon changes every hour or more frequently
- Severe cramping that interferes with daily activities
- Bleeding or spotting between periods
- Absence of periods for three months or more in individuals who are not pregnant
- Sudden changes in previously regular cycles
These symptoms may indicate conditions such as hormonal imbalances, fibroids, endometriosis, or other reproductive health issues that benefit from medical intervention.
Lifestyle Factors Affecting the Menstrual Cycle
Various lifestyle factors can influence menstrual cycle regularity and characteristics. Stress, significant weight changes, excessive exercise, and certain medical conditions can all affect hormonal balance and menstrual patterns.
Stress and Hormones
Chronic stress can disrupt the delicate hormonal balance required for regular menstrual cycles. Stress hormones can interfere with the production and release of reproductive hormones, potentially causing irregular periods or even temporary cessation of menstruation.
Weight and Exercise
Both very low body weight and obesity can affect menstrual regularity. Extremely low body fat percentages may cause periods to stop entirely, while obesity can lead to irregular cycles due to hormonal imbalances. Similarly, excessive exercise, particularly when combined with low caloric intake, can disrupt normal menstrual function.
Conclusion
Understanding the menstrual cycle empowers individuals to take charge of their reproductive health. By recognizing normal patterns