Understanding Testicular Torsion: Causes, Symptoms, and Emergency Treatment
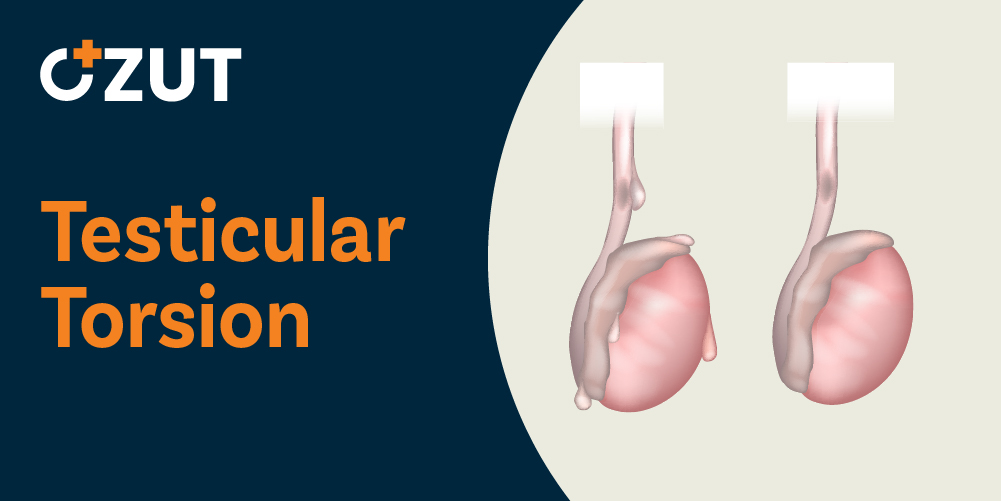
Testicular torsion represents a critical medical emergency that requires immediate attention. This condition occurs when the tissues surrounding the testicle fail to attach properly, allowing the organ to twist around the spermatic cord. This twisting motion restricts blood flow to the affected testicle, leading to severe pain and swelling. Understanding the signs, symptoms, and treatment options for this condition can help individuals recognize when emergency medical care becomes necessary.
Normal Anatomy and Function of the Male Reproductive System
The male reproductive system includes two testicles that hang within a protective pouch of skin called the scrotum, positioned below the penis. These organs serve two primary functions: producing sperm cells and generating testosterone, the primary male sex hormone. Each testicle receives its blood supply through the spermatic cord, a vital structure that originates in the abdomen and extends downward into the scrotum.
The spermatic cord contains multiple important components beyond blood vessels. It houses the vas deferens, a tube responsible for transporting sperm from the testicles to the urethra during ejaculation. This complex network of vessels and ducts must remain unobstructed to maintain proper testicular function and overall reproductive health.
Under normal circumstances, both testicles should appear approximately equal in size. The tissue surrounding each testicle typically provides adequate support and attachment to prevent abnormal movement or rotation within the scrotal sac.
Recognizing the Warning Signs and Symptoms
The hallmark symptom of testicular torsion manifests as sudden, severe pain concentrated on one side of the scrotum. This pain typically develops without warning and increases in intensity rapidly. Individuals experiencing this condition often describe the discomfort as sharp, stabbing, or crushing in nature.
Physical Changes in the Scrotum
Beyond pain, several visible changes may indicate testicular torsion. The affected side of the scrotum may quickly enlarge, becoming noticeably larger than the opposite side. Color changes represent another critical warning sign, with the scrotal skin potentially turning red or developing a darker appearance. Initially, swelling might not be present, but within a short timeframe, the scrotal skin typically becomes swollen and reddened.
Associated Symptoms
Many individuals with testicular torsion experience additional symptoms beyond localized pain. Nausea and vomiting frequently accompany the condition, likely resulting from the severe pain and the body’s stress response. Some patients report difficulty finding a comfortable position, constantly shifting or adjusting their posture in an attempt to alleviate discomfort.
In less common presentations, testicular torsion may develop gradually over several hours or days, with pain increasing slowly rather than appearing suddenly. However, symptoms such as burning during urination or increased urinary frequency do not typically indicate torsion and may suggest alternative conditions.
Understanding the Urgency of Treatment
Testicular torsion qualifies as a true medical emergency because the twisted spermatic cord completely cuts off blood supply to the affected testicle. Without adequate blood flow, testicular tissue begins to deteriorate rapidly. Medical research indicates that permanent damage begins after approximately six hours of interrupted blood supply.
When blood flow remains blocked, the testicle undergoes a process called atrophy, where the organ shrinks and loses function. If blood supply is not restored promptly, the tissue dies in a process known as infarction. A dead testicle causes the scrotum to become extremely tender, red, and swollen, with patients experiencing severe, unrelenting discomfort.
Studies demonstrate that surgical intervention delayed beyond twelve hours results in testicle removal in nearly three out of four cases. This statistic underscores the critical importance of seeking immediate medical attention when symptoms appear.
Risk Factors and Occurrence Patterns
Testicular torsion affects approximately one in four thousand males under age twenty-five, though it can occur in newborns and older men as well. The condition develops more frequently on the left side compared to the right, and bilateral torsion affecting both testicles simultaneously occurs in only two percent of cases, primarily in newborn infants.
Anatomical Predisposition
Most males possess tissue that firmly attaches the testicles to the scrotum, preventing abnormal rotation. However, some individuals are born with inadequate tissue attachment, allowing the testicles to move freely within the scrotal sac. This anatomical variation, sometimes referred to as a bell clapper deformity, significantly increases torsion risk.
Importantly, physical activity does not cause testicular torsion. The condition may occur during exercise, but it can equally develop while sitting, standing, or sleeping. This unpredictability emphasizes that lifestyle modifications cannot prevent torsion in anatomically predisposed individuals.
Diagnostic Procedures and Medical Evaluation
Healthcare providers typically diagnose testicular torsion through physical examination combined with imaging studies. During the physical exam, the physician assesses scrotal swelling, tenderness, and testicle position. However, physical examination alone may not provide definitive diagnosis.
Ultrasound imaging serves as the primary diagnostic tool for confirming testicular torsion. This non-invasive procedure allows medical professionals to visualize blood flow to the testicles, identifying areas where circulation has been compromised. The ultrasound can differentiate torsion from other conditions that cause testicular pain, such as infections of the testicle or epididymis.
Because infection represents an alternative cause of testicular pain, urine testing may be performed to rule out urinary tract infections or other infectious processes. This comprehensive diagnostic approach ensures accurate identification of the underlying problem.
Surgical Treatment and Emergency Intervention
All patients with confirmed testicular torsion require surgical treatment. While emergency room physicians may attempt to manually untwist the spermatic cord, surgery remains necessary to prevent recurrence. Urological specialists perform the definitive surgical procedure to address this condition.
Surgical Procedure Details
During surgery, the urologist untwists the spermatic cord to restore blood flow, a process called detorsion. After untwisting the cord, the surgeon places permanent stitches to secure the testicle in position, preventing future torsion episodes. Most procedures are performed through an incision in the scrotum, though some cases require a groin incision.
If the testicle cannot be saved due to prolonged blood flow interruption, the surgeon removes the affected organ through a procedure called orchidectomy. Even when removal becomes necessary, the surgeon still places preventive stitches around the remaining testicle to protect against future torsion on that side.
Special Considerations for Newborns
Testicular torsion in newborns presents unique challenges. The affected testicle is rarely salvageable, as tissue death typically occurs before or during birth. Emergency surgery in infants differs from adult procedures due to concerns about anesthesia and the risk of torsion developing in the opposite testicle shortly after birth.
Modern pediatric urology practices increasingly favor early surgical intervention within the first few hours or days of life. This approach allows removal of the non-viable testicle while placing protective stitches around the healthy testicle to prevent bilateral loss.
Recovery Process and Post-Operative Care
Surgical treatment for testicular torsion requires a recovery period for proper healing. Patients typically need pain medication for several days following the procedure. Most individuals can return to work or school within one week, though the exact timeline varies based on individual healing rates and the extent of surgery performed.
Strenuous physical activity and vigorous exercise should be avoided for several weeks following surgery. This restriction allows adequate healing time and reduces the risk of complications. The internal stitches placed around the testicle should not cause noticeable discomfort and remain permanently in place to prevent future torsion.
Potential Long-Term Changes
Even when the twisted testicle is successfully saved, some degree of shrinkage may occur due to damage sustained during the period of reduced blood flow. When one testicle is removed, the remaining testicle may undergo compensatory hypertrophy, growing larger than normal to maintain adequate hormone production and sperm generation.
Impact on Fertility and Reproductive Function
A single healthy testicle can produce normal quantities of sperm and testosterone, maintaining fertility and typical male characteristics. However, research indicates that up to one-third of patients experience reduced sperm counts following testicular torsion, even when the testicle is preserved.
Testicular torsion can trigger the production of anti-sperm antibodies, proteins that may interfere with sperm function and motility. While some studies suggest these factors could reduce fertility, significant fertility problems remain relatively uncommon. Most men with one healthy testicle maintain normal reproductive capability.
Lifestyle Considerations After Testicular Loss
Individuals who have lost a testicle or have a weakened testicle should take precautions to protect the remaining organ. Wearing protective equipment during contact sports becomes essential to prevent injury. Any unusual discomfort or abnormalities in the scrotum warrant immediate medical evaluation.
Some men may experience decreased testosterone levels at an earlier age than typical. Regular monitoring of testosterone levels as individuals age helps identify and address hormonal deficiencies before they cause significant symptoms or health problems.
Testicular Prosthesis Options
Men who have undergone testicle removal may consider a testicular prosthesis to restore normal appearance and feel. These devices, typically made of silicone and filled with saline solution, are usually implanted after the patient has completed puberty and reached full physical maturity.
Placing a prosthesis in young boys requires consideration of future growth. A smaller prosthesis suitable for a child would need replacement with an adult-sized device later, necessitating additional surgery. Prosthesis placement typically occurs several months after testicle removal, allowing adequate healing time. The decision to pursue prosthetic implantation remains personal and should be discussed thoroughly with a urological specialist.
Related Torsion Conditions
Other types of torsion can affect structures near the testicle. Torsion of the appendix of the epididymis or appendix of the testicle involves twisting of small, vestigial structures attached to these organs. These embryonic remnants serve no function in adult males but can undergo torsion, causing tissue death in the affected appendage.
This alternative form of torsion occurs more commonly in prepubescent boys than true testicular torsion and rarely affects older adolescents or adult men. While less severe than testicular torsion, these conditions still require medical evaluation and appropriate treatment.
Prevention and Ongoing Monitoring
No lifestyle modifications or medications can prevent testicular torsion in anatomically predisposed individuals. Only surgical placement of permanent stitches provides reliable prevention. Men who have experienced torsion on one side should remain vigilant for symptoms affecting the opposite testicle, though surgical fixation during the initial procedure significantly reduces this risk.
Any scrotal pain, swelling, or unusual changes warrant immediate medical attention, even in the absence of obvious swelling or skin discoloration. Early recognition and prompt treatment maximize the chances of preserving testicular function and preventing long-term complications. Understanding the signs of testicular torsion empowers individuals to seek timely care when this urological emergency occurs.