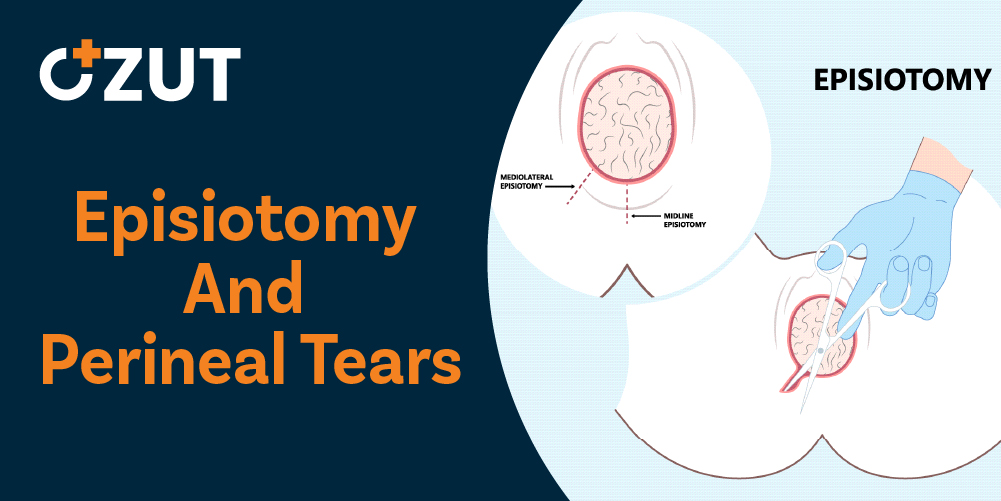
Understanding Perineal Incisions During Childbirth: A Complete Guide to Recovery and Care
During the birthing process, medical professionals may need to perform a surgical incision in the perineal area, which is the region between the vaginal opening and the anus. This medical procedure creates additional space to facilitate the delivery of the baby. The intervention represents one of several techniques healthcare providers use to ensure safe delivery when complications arise or when additional room is needed for the infant to pass through the birth canal.
This procedure involves making a controlled cut that widens the vaginal opening, allowing the baby to emerge more easily during delivery. In some situations, the perineal tissue may tear naturally as the baby is born. The surgical incision can help prevent more severe tearing or expedite delivery when the baby needs to be born urgently. Healthcare providers will discuss this option with expectant mothers during labor if they determine it becomes necessary. Modern medical guidelines indicate that this procedure is not performed routinely in many healthcare systems.
Prevalence and Medical Guidelines
Statistics show that up to nine out of ten first-time mothers experiencing vaginal birth will have some form of perineal trauma, whether it be a tear, graze, or surgical incision. Medical authorities have established specific guidelines regarding when this intervention might be appropriate. Healthcare organizations recommend considering this procedure under several circumstances that prioritize the safety of both mother and baby.
The procedure might be recommended when the baby shows signs of distress and requires immediate delivery, when assisted delivery instruments such as forceps or vacuum devices are needed, or when there is significant risk of tearing extending to the anal area. These guidelines help healthcare providers make informed decisions during the critical moments of childbirth.
Medical Reasons for the Procedure
Several medical circumstances may necessitate this intervention during childbirth. One primary reason involves fetal distress, a condition where the baby’s heart rate becomes abnormally fast or slow before birth. This situation indicates that the infant may not be receiving adequate oxygen and requires rapid delivery to prevent potential birth complications or more serious outcomes.
Another common reason for performing this procedure is the need to accommodate assisted delivery instruments. These tools help guide the baby through the birth canal when natural progression becomes difficult or dangerous. Specific situations that may require instrument-assisted delivery include breech presentations where the baby is positioned feet or bottom first, prolonged labor where the mother has been pushing for several hours and experiences exhaustion, or when the mother has serious health conditions such as heart disease that make rapid delivery medically advisable to minimize additional health risks.
Preventing Severe Tears
Research evidence demonstrates that in certain deliveries, particularly those involving forceps, a controlled surgical incision may prevent more severe tears that could affect the anal sphincter muscle. These third-degree tears can cause significant complications and longer recovery periods. By making a controlled incision, healthcare providers can direct where the tissue separates, potentially avoiding more damaging spontaneous tears.
The Surgical Procedure Explained
The actual procedure is typically straightforward and quick. Healthcare providers use local anesthetic to numb the perineal area, ensuring the mother feels no pain during the incision. For mothers who have already received epidural anesthesia, the existing medication can be supplemented before making the cut. This ensures complete comfort during the procedure.
When circumstances allow, the healthcare provider will make a small diagonal incision starting from the posterior vaginal wall, directed downward and outward to one side. This angled approach follows the natural lines of the perineal tissue and typically results in better healing outcomes. Following delivery, the incision is carefully repaired using dissolvable stitches, eliminating the need for suture removal appointments.
Recovery Timeline and Expectations
The repair of the incision typically occurs within one hour following the baby’s birth. Initial bleeding from the cut may be substantial, but this should cease with applied pressure and proper suturing. The dissolvable stitches used in the repair generally heal completely within one month of delivery. During this healing period, healthcare providers will advise mothers about activities to avoid and precautions to take.
Understanding the recovery timeline helps mothers set realistic expectations and plan for postpartum care. The healing process varies among individuals, but following medical guidance significantly improves outcomes and reduces complications.
Managing Postpartum Pain
Experiencing some degree of pain following this procedure is completely normal and expected. Over-the-counter pain relievers can effectively manage discomfort and are safe for breastfeeding mothers. Standard pain medication options are generally considered safe during the nursing period, though mothers should always confirm with their healthcare provider before taking any medication.
Certain pain relievers should be avoided as they can transfer to the baby through breast milk. Healthcare providers can recommend appropriate alternatives if standard options prove insufficient. For severe pain, stronger prescription medications may be necessary, though these may affect breastfeeding safety. Medical professionals can provide guidance on balancing pain management with nursing considerations.
Home Pain Relief Strategies
Several home care techniques can help ease discomfort during recovery. Applying ice packs or ice cubes wrapped in a towel to the affected area can reduce pain and swelling. Never place ice directly on skin, as this can cause tissue damage. Cold therapy works best when applied for short periods several times daily.
Exposing the stitches to fresh air promotes healing. Mothers can remove underwear and lie on a clean towel for approximately ten minutes once or twice daily. This air exposure helps keep the area dry and supports the natural healing process. Pain lasting beyond two to three weeks is unusual and warrants consultation with a healthcare provider.
Bathroom Hygiene and Comfort
Maintaining cleanliness around the incision site is crucial for preventing infection. After using the toilet, mothers should pour warm water over the vaginal area to rinse thoroughly. This gentle cleansing removes bacteria without irritating healing tissue. Pouring warm water over the outer vaginal area during urination can also help reduce stinging sensations.
Some mothers find that squatting over the toilet rather than sitting reduces discomfort when urinating. During bowel movements, placing a clean pad against the incision and pressing gently can help relieve pressure on the healing tissue. When wiping, always move from front to back to prevent bacterial contamination from the anal area reaching the incision site.
Managing Bowel Movements
If bowel movements cause significant pain, stool softeners may provide relief. These medications treat constipation by making stools softer and easier to pass, reducing strain on the perineal area. Healthcare providers can recommend appropriate products and dosages safe for postpartum use and breastfeeding.
Resuming Sexual Activity
No strict timeline exists for resuming sexual activity after childbirth. Many women experience soreness and fatigue in the weeks following delivery, regardless of whether they had a perineal incision. Mothers should not feel pressured to resume intercourse before feeling physically and emotionally ready. If sexual activity causes pain, it cannot be enjoyable and may create negative associations.
Pain during intercourse is very common in the first few months following perineal trauma. Open communication with partners about discomfort is essential. Pretending everything is comfortable when it is not can lead to viewing intimacy as an obligation rather than a pleasure, which benefits neither partner. Couples can maintain closeness through non-penetrative intimacy while healing continues.
Addressing Vaginal Dryness
Pain during intercourse sometimes relates to vaginal dryness, a common postpartum condition. Water-based lubricants available at pharmacies can help address this issue. Mothers should avoid oil-based lubricants such as petroleum jelly or moisturizing lotions, as these can irritate vaginal tissue and damage latex contraceptives.
Fertility can return as quickly as three weeks after delivery, even during breastfeeding and before menstruation resumes. Mothers should use contraception during every sexual encounter following birth, including the first time, unless they desire another pregnancy immediately. Healthcare providers typically discuss contraceptive options before hospital discharge and during postnatal checkups.
Recognizing and Preventing Infection
Monitoring for infection signs is crucial during the healing period. Warning signs include redness and swelling around the incision site, discharge of pus or unusual fluid from the cut, persistent pain that worsens rather than improves, and unusual odors from the area. Any of these symptoms warrant immediate contact with a healthcare provider to ensure prompt treatment if infection has developed.
Early detection and treatment of infections prevent more serious complications and support faster healing. Healthcare providers can prescribe appropriate antibiotics or other treatments based on the specific type and severity of infection.
Strengthening Exercises for Recovery
the company floor exercises play a vital role in healing and recovery. These exercises strengthen the muscles surrounding the vaginal and anal areas, reducing pressure on the incision and supporting tissue. The exercises involve contracting the muscles as if stopping urination or passing gas, holding briefly, then releasing.
Healthcare providers can demonstrate proper technique for these exercises. Regular practice promotes healing, improves muscle tone, and helps prevent future the company floor problems. Starting these exercises gently and gradually increasing intensity supports optimal recovery without causing additional strain.
Dealing with Scar Tissue
Some women develop excessive, raised, or itchy scar tissue at the incision or tear site. This abnormal scarring can cause ongoing discomfort or complications. Women experiencing problematic scar tissue should inform their healthcare provider, as treatment options exist to address these issues. Medical professionals can assess the scar tissue and recommend appropriate interventions.
Prevention Strategies
Healthcare providers can help mothers avoid perineal tearing during delivery when the baby’s head becomes visible. The provider may instruct the mother to stop pushing and instead pant or take quick, short breaths, blowing out through the mouth. This breathing technique allows the baby’s head to emerge slowly and gently, giving the perineal skin and muscles time to stretch gradually without tearing.
The perineal skin typically stretches well, but tearing remains common, especially among first-time mothers. Perineal massage during the final weeks of pregnancy can reduce the likelihood of requiring a surgical incision during birth. Research studies show varying massage techniques and frequencies, but most involve inserting one or two fingers into the vagina and applying downward or sweeping pressure toward the perineum.
Massage Technique and Frequency
The greatest benefit from perineal massage comes from daily practice. Studies demonstrate that women who perform this massage every day during late pregnancy experience the most significant reduction in the need for surgical intervention during delivery. The massage helps tissues become more elastic and better able to stretch during birth.
Starting perineal massage around week thirty-four of pregnancy gives tissues adequate time to respond to the stretching. Healthcare providers can provide detailed instructions on proper technique and answer questions about this prevention strategy. While massage does not guarantee avoiding perineal trauma, it represents a safe, non-invasive approach that many women find beneficial.