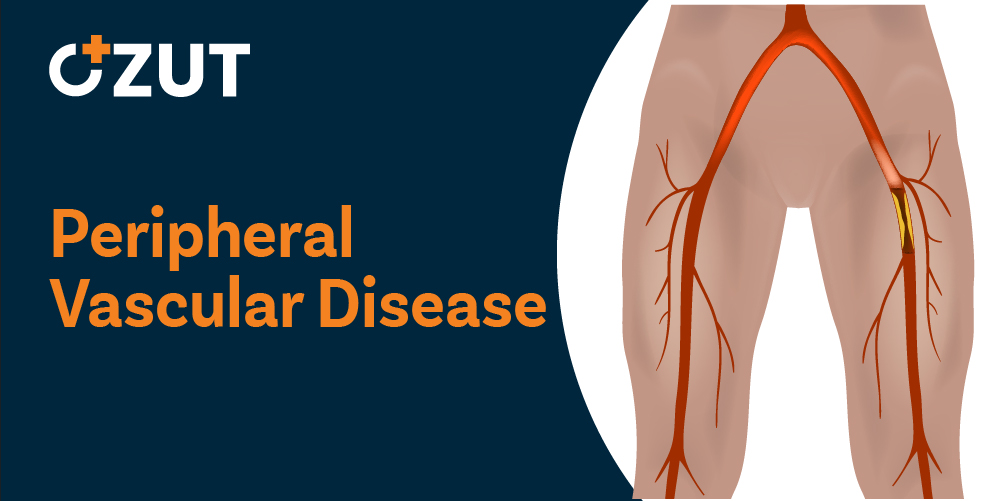
Understanding Circulatory Disorders: Causes, Symptoms, and Treatment Options
Circulatory disorders affecting the extremities represent a significant health concern that impacts millions of people worldwide. These conditions develop gradually over time and involve the narrowing, blockage, or spasms of blood vessels that supply vital organs and tissues throughout the body. Understanding these disorders is essential for early detection, proper management, and prevention of serious complications.
What Are Circulatory Disorders of the Extremities
Circulatory disorders affecting the extremities are progressive conditions that impact blood vessels outside the heart. These disorders can affect arteries, veins, and lymphatic vessels, potentially compromising blood flow to various organs and tissues. When blood vessels become narrowed or blocked, the affected areas may not receive adequate blood flow necessary for healthy tissue function and maintenance.
The legs and feet are the most commonly affected areas, though these conditions can impact any part of the body supplied by blood vessels outside the heart. The progressive nature of these disorders means that symptoms typically worsen over time if left untreated, making early intervention crucial for optimal outcomes.
Primary Causes and Contributing Factors
The development of circulatory disorders stems from various underlying causes, with some being more common than others. Understanding these causes helps healthcare providers develop targeted treatment strategies and helps patients make informed decisions about their health management.
Plaque Buildup and Arterial Narrowing
The most prevalent cause of circulatory disorders in the extremities is the accumulation of plaque within arterial walls. This process involves the gradual buildup of fatty deposits, cholesterol, and other substances that adhere to the inner walls of arteries. As plaque accumulates, it reduces the internal diameter of blood vessels, restricting blood flow to the limbs and decreasing the delivery of oxygen and essential nutrients to tissues.
Blood clots can form on top of existing plaque deposits, further reducing the available space within blood vessels. In severe cases, these clots can completely block major arteries, leading to critical reductions in blood flow and potentially life-threatening complications.
Additional Contributing Factors
Beyond plaque accumulation, several other factors can contribute to the development of circulatory disorders:
- Physical trauma or injury to the arms or legs that damages blood vessels
- Anatomical irregularities in muscles or ligaments that compress blood vessels
- Infections that affect the company tissue
- Concurrent heart conditions that affect overall circulatory function
Research indicates a strong correlation between coronary heart conditions and circulatory disorders of the extremities, suggesting that individuals with heart disease face elevated risks for developing the company problems in their limbs.
Risk Factors and Vulnerable Populations
Certain factors increase the likelihood of developing circulatory disorders. These risk factors fall into two categories: those that cannot be modified and those that can be addressed through lifestyle changes or medical intervention.
Non-Modifiable Risk Factors
Some risk factors are inherent and cannot be changed through intervention. These include advancing age, particularly for individuals over fifty years old, biological sex with males facing higher risk, the company status in women, personal history of heart conditions, and the company history of high cholesterol, elevated blood pressure, or the company diseases. Understanding these unchangeable factors helps healthcare providers assess individual risk levels and implement appropriate monitoring strategies.
Modifiable Risk Factors
Many risk factors can be addressed through lifestyle modifications and medical treatment. These controllable factors include existing coronary heart disease, diabetes mellitus, elevated cholesterol levels, high blood pressure, excess body weight, sedentary lifestyle, and tobacco use in any form. Individuals who smoke or have diabetes face particularly high risks for complications because these conditions significantly impair blood flow throughout the body.
Recognizing Symptoms and Warning Signs
Approximately half of all individuals with circulatory disorders experience no noticeable symptoms, making regular health screenings essential for early detection. For those who do experience symptoms, recognizing warning signs enables prompt medical intervention.
Primary Symptom: Exercise-Related Leg Pain
The most common initial symptom is painful cramping in the legs that occurs during physical activity and subsides with rest. This condition occurs because muscles require increased blood flow during exercise, but narrowed arteries cannot deliver adequate blood supply. During rest periods, muscle oxygen demands decrease, allowing pain to resolve. This cramping may affect one or both legs depending on the location and extent of arterial narrowing.
Additional Warning Signs
Beyond exercise-related cramping, numerous other symptoms may indicate circulatory problems:
- Skin changes including decreased temperature, thinness, brittleness, or unusual shininess on legs and feet
- Diminished or absent pulses in the lower extremities
- Tissue death resulting from severe blood flow restriction
- Hair loss on affected limbs
- Sexual dysfunction in men
- Non-healing wounds over pressure points such as heels and ankles
- Numbness, weakness, or heaviness in leg muscles
- Burning or aching pain at rest, particularly in toes and during nighttime
- Paleness when legs are elevated above heart level
- Reddish-blue discoloration of extremities
- Limited range of motion and mobility
- Severe pain indicating critical arterial narrowing or complete blockage
- Thickened, opaque toenails
Because these symptoms can overlap with other medical conditions, professional medical evaluation is essential for accurate diagnosis and appropriate treatment planning.
Diagnostic Procedures and Testing Methods
Healthcare providers employ various diagnostic tools to confirm circulatory disorders and assess their severity. These tests provide detailed information about blood flow, vessel condition, and the extent of blockages.
Imaging and Visualization Techniques
Advanced imaging procedures allow healthcare providers to visualize blood vessels and identify areas of narrowing or blockage. One common method involves injecting contrast dye through a thin, flexible tube inserted into a leg artery, making blood vessels visible on X-ray images. This technique helps pinpoint exact locations and severity of blockages.
Another noninvasive imaging approach uses powerful magnets, radio waves, and computer technology to create detailed images of blood vessels and surrounding tissues. A special dye enhances vessel visibility during this procedure, providing comprehensive views of the company anatomy.
Blood Pressure Comparison Tests
Comparing blood pressure measurements between different body locations helps assess blood flow adequacy. Healthcare providers measure blood pressure in the ankle and arm, then calculate a ratio by dividing ankle pressure by arm pressure. This comparison reveals whether blood flow to the lower extremities is compromised.
Similar tests use tiny blood pressure cuffs around toes combined with infrared light sensors to evaluate blood flow near the skin surface. These measurements are then compared to arm blood pressure readings to identify circulation problems.
Ultrasound and Flow Studies
High-frequency sound waves combined with computer processing create images of blood vessels and assess blood flow patterns. Healthcare providers use specialized equipment to measure and evaluate circulation, with faint or absent sounds indicating blocked blood flow. This noninvasive technique provides valuable information about vessel function without requiring contrast dyes or radiation exposure.
Exercise and Stress Testing
Walking on a treadmill while healthcare providers monitor blood flow helps assess how circulation responds to physical activity demands. For patients unable to walk on treadmills, alternative tests involve taking comparative blood pressure measurements at different leg locations while lying down, revealing circulation deficiencies between measurement sites.
Advanced Waveform Analysis
Specialized recording devices measure blood volume changes in the legs and display results as waveforms. Healthcare providers analyze these patterns to assess circulation quality and identify areas of restricted blood flow. This technique provides detailed information about how blood moves through vessels during different phases of the cardiac cycle.
Treatment Approaches and Management Strategies
Treatment for circulatory disorders focuses on controlling symptoms and preventing disease progression. These goals are critical for reducing risks of heart attack, stroke, and other serious complications. Treatment plans typically combine multiple approaches tailored to individual patient needs.
Lifestyle Modifications
Fundamental to managing circulatory disorders are lifestyle changes that address controllable risk factors. Regular physical exercise improves circulation and helps maintain healthy blood vessels. Proper nutrition supports the company health and helps control weight, cholesterol, and blood sugar levels. Complete cessation of tobacco use is essential, as smoking severely impairs blood flow and accelerates disease progression.
Medical Management of Contributing Conditions
Aggressive treatment of conditions that worsen circulatory disorders is crucial for preventing complications. This includes rigorous control of diabetes through medication, diet, and lifestyle modifications. Managing high blood pressure and elevated cholesterol levels through appropriate medications and lifestyle changes helps slow disease progression and reduces cardiovascular risks.
Pharmaceutical Interventions
Various medications help improve blood flow and prevent complications. Antiplatelet agents reduce blood clot formation, while medications that relax blood vessel walls help improve circulation. Healthcare providers select specific medications based on individual patient characteristics, disease severity, and concurrent medical conditions.
Surgical and Interventional Procedures
When conservative treatments prove insufficient, surgical interventions may become necessary. Bypass surgery involves using a blood vessel from another body location or a synthetic tube to reroute blood flow around blocked or narrowed arteries. This procedure restores adequate blood supply to affected tissues.
Less invasive procedures involve inserting thin, flexible tubes into blood vessels to widen narrowed areas and improve blood flow. Several techniques accomplish this goal:
- Inflating small balloons inside blocked arteries to compress plaque and widen the vessel opening
- Using tiny cutting devices to remove plaque buildup from arterial walls
- Employing laser technology to vaporize blockages
- Placing expandable metal coils inside arteries to hold them open permanently
Healthcare providers may perform imaging studies before surgical procedures to precisely locate blockages and plan optimal treatment approaches.
Potential Complications and Long-Term Outcomes
Complications from circulatory disorders typically result from severely decreased or absent blood flow to affected tissues. Understanding these potential complications emphasizes the importance of early intervention and consistent treatment adherence.
Severe complications may include limb amputation when tissue death becomes extensive, poor wound healing due to inadequate blood supply, restricted mobility caused by pain and discomfort, severe pain in affected extremities, and significantly increased stroke risk. Research indicates that individuals with circulatory disorders face three times higher stroke risk compared to those without these conditions.
Following an aggressive, comprehensive treatment plan significantly reduces complication risks and improves long-term outcomes. Regular monitoring and prompt attention to worsening symptoms enable healthcare providers to adjust treatments before serious complications develop.
Prevention Strategies and Risk Reduction
Preventing circulatory disorders or slowing their progression requires addressing modifiable risk factors through comprehensive lifestyle changes and medical management. A thorough prevention program encompasses multiple components working together to maintain the company health.
Tobacco Cessation
Complete elimination of tobacco use in all forms represents the single most important preventive measure. This includes quitting smoking, avoiding secondhand smoke exposure, and discontinuing use of all tobacco products. Tobacco use severely damages blood vessels and dramatically accelerates disease progression.
Dietary Modifications
Nutritional changes play a crucial role in preventing and managing circulatory disorders. Effective dietary strategies include reducing intake of fats, cholesterol, and