Understanding Autoimmune Eye Disease: A Comprehensive Guide to Ocular Blistering Disorders
Autoimmune conditions affecting the eyes represent some of the most challenging disorders in ophthalmology. When the immune system mistakenly attacks the delicate tissues of the eye, particularly the mucous membranes, the consequences can be severe and life-altering. This comprehensive guide explores a specific autoimmune condition that affects the ocular surface, causing progressive scarring and potentially devastating vision loss if left untreated.
What Are Autoimmune Blistering Disorders of the Eye
Autoimmune blistering disorders affecting the eye belong to a broader category of conditions where the body’s immune system attacks its own tissues. These disorders specifically target mucous membranes throughout the body, creating painful blistering lesions that can appear in multiple locations simultaneously. The condition represents a subset of rare autoimmune diseases that require specialized medical attention and long-term management.
The ocular manifestation of this disorder stands out as particularly serious among the various forms. While the condition can affect multiple body systems, the eye involvement presents unique challenges due to the delicate nature of ocular tissues and the critical importance of vision to quality of life. Understanding the mechanisms, symptoms, and treatment options for this condition is essential for patients, caregivers, and healthcare providers alike.
The Scope and Impact of Mucous Membrane Autoimmune Conditions
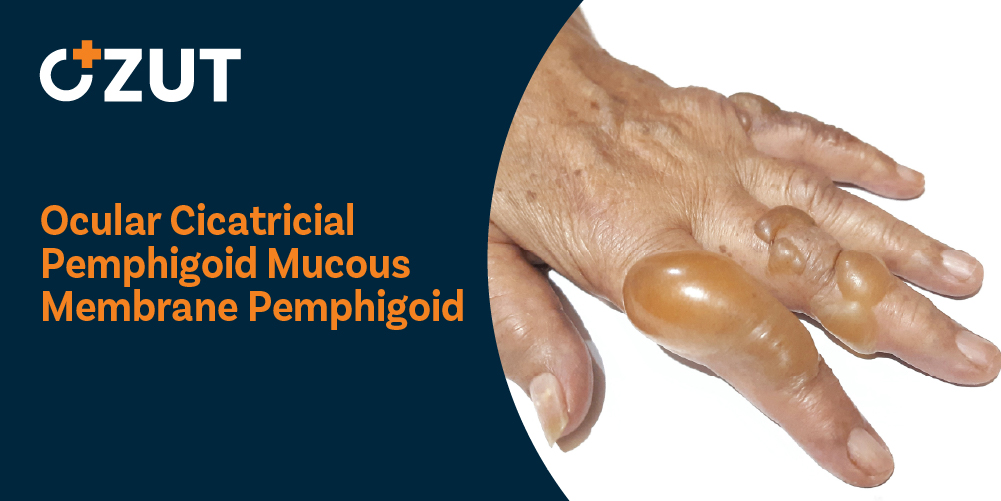
This autoimmune disorder affects various mucous membranes throughout the body, creating a complex clinical picture that requires comprehensive medical management. The condition can manifest in several anatomical locations, each presenting its own set of challenges and symptoms. Common sites of involvement include the oral cavity, where the gums and inner cheek lining may develop blistering lesions. The nasal passages, throat, and genital areas can also be affected, along with the anus and skin surfaces.
The distribution and severity of symptoms vary significantly among individuals. Some patients may experience mild involvement limited to one or two sites, while others face more extensive disease affecting multiple body systems simultaneously. This variability makes diagnosis and treatment planning particularly challenging, requiring careful evaluation by specialists familiar with autoimmune disorders.
Why Eye Involvement Demands Special Attention
When this autoimmune condition affects the eyes, the stakes become considerably higher. The ocular form of the disease carries a particularly grave prognosis if medical intervention is delayed or inadequate. Statistical data reveals the serious nature of untreated ocular involvement, with bilateral blindness occurring in approximately one-fifth of cases and severe vision impairment affecting nearly one-third of affected eyes.
The progressive nature of the ocular disease means that early detection and aggressive treatment are paramount. Unlike some forms of the condition that may follow a more benign course, the eye manifestation tends to worsen over time without appropriate therapeutic intervention. This progression underscores the critical importance of prompt diagnosis and initiation of treatment protocols designed to preserve vision and prevent irreversible damage to ocular structures.
Understanding the Disease Mechanism
The precise cause of this autoimmune blistering disorder remains an area of active research. Scientists have identified several key factors that contribute to disease development and progression. The fundamental problem lies in immune system dysfunction, where the body’s defense mechanisms mistakenly identify healthy tissues as foreign threats requiring elimination.
Research has revealed the presence of autoantibodies, which are antibodies that target the body’s own proteins rather than external pathogens. These autoantibodies play a central role in the disease process by attacking specific components of mucous membrane tissues. Additionally, autoreactive T cells, which are immune cells that have escaped normal regulatory mechanisms, contribute to the inflammatory cascade that leads to tissue damage and blister formation.
Complex Patterns of Disease Activity
One of the most puzzling aspects of this condition involves the complex mechanisms governing disease activation and remission. The disorder does not follow a predictable linear course. Instead, patients may experience periods of active disease alternating with phases of relative quiescence. Understanding what triggers these fluctuations remains an important research priority, as such knowledge could lead to more effective preventive strategies and treatment approaches.
The condition can emerge at various life stages, though certain age groups face higher risk. Most commonly, the disorder manifests during middle to later adulthood, typically between the ages of forty and seventy years. However, cases outside this age range do occur, highlighting the importance of maintaining clinical suspicion across all age groups when characteristic symptoms present.
Recognizing the Signs and Symptoms
Early recognition of ocular autoimmune disease symptoms is crucial for timely intervention and vision preservation. The condition produces a constellation of signs and symptoms that reflect progressive damage to ocular surface structures. Patients and healthcare providers must remain vigilant for these warning signs to ensure prompt diagnosis and treatment initiation.
Common Ocular Manifestations
The earliest symptoms often involve changes in how the eye feels and functions. Many patients report a sensation of roughness on the inside of their eyelids, as if something is constantly irritating the eye surface. This roughness results from inflammatory changes and early scarring of the conjunctival tissue that lines the inner eyelid.
A persistent gritty sensation frequently accompanies the roughness, making patients feel as though sand or small particles are trapped in their eyes. This symptom can be particularly bothersome and may worsen throughout the day. Redness of the eye is another common finding, reflecting the ongoing inflammatory process affecting ocular tissues. Pain may also develop, ranging from mild discomfort to severe aching that significantly impacts quality of life.
Progressive Structural Changes
As the disease advances, more dramatic structural changes become apparent. The eyelashes may begin turning inward, a condition that causes them to rub against the cornea with each blink. This misdirection of lashes creates additional trauma to an already compromised ocular surface. Similarly, the eyelids themselves may turn inward, further exacerbating surface irritation and damage.
One of the hallmark features of advanced disease involves shrinking of the space between the eyeball and eyelid. This occurs as scarring tissue contracts, pulling structures closer together and restricting normal eye movement. In severe cases, abnormal adhesions may form between the eyeball and eyelid, creating partial or complete attachment. This complication, known as symblepharon, represents a serious development that can severely limit eye mobility and function.
Advanced Disease Manifestations
In the most severe cases, the eye’s surface undergoes dramatic transformation. The normally transparent and smooth ocular surface may thicken and take on a skin-like appearance, a process called keratinization. This change fundamentally alters the optical properties of the eye and can lead to significant vision problems. When disease progression reaches this stage, affected eyes face substantial risk of permanent vision loss, making aggressive treatment essential.
Diagnostic Approaches and Evaluation
Accurate diagnosis of this autoimmune eye condition requires a systematic and thorough evaluation. When healthcare providers suspect the disorder based on clinical presentation, they initiate a comprehensive ophthalmologic assessment designed to confirm the diagnosis and evaluate disease extent. This evaluation serves as the foundation for treatment planning and prognostic assessment.
Comprehensive Eye Examination
The diagnostic process begins with a detailed examination of all ocular structures. Specialists use various instruments and techniques to assess the health of the conjunctiva, cornea, eyelids, and other relevant tissues. This examination looks for characteristic signs of the disease, including inflammation, scarring, and structural abnormalities. The evaluation also assesses visual function to determine whether the disease has already impacted vision.
Special attention is paid to the conjunctiva, the thin membrane covering the white part of the eye and lining the inner eyelids. This tissue often shows the earliest signs of disease activity and provides valuable diagnostic information. Specialists examine the conjunctiva for evidence of inflammation, blister formation, and scarring patterns characteristic of autoimmune blistering disorders.
Tissue Biopsy and Laboratory Analysis
Definitive diagnosis typically requires tissue biopsy, a procedure in which a small sample of affected tissue is removed for microscopic examination. The biopsy may be taken from the conjunctiva of the eye or, in some cases, from the gums if oral involvement is present. This tissue sample undergoes specialized laboratory testing designed to detect the presence of autoantibodies and characteristic pathological changes.
The biopsy specimen is examined using various techniques, including direct immunofluorescence, which can reveal the presence and pattern of antibody deposits in the tissue. These findings help confirm the diagnosis and distinguish this condition from other disorders that may produce similar clinical appearances. Laboratory analysis provides crucial information that guides treatment decisions and helps predict disease behavior.
Treatment Strategies and Management Approaches
Managing this autoimmune eye condition requires a multifaceted approach that addresses both the underlying immune dysfunction and the local ocular complications. Treatment strategies have evolved significantly over recent decades, with modern protocols achieving success rates approaching ninety percent in controlling disease activity. However, the serious risk of vision loss demands aggressive intervention, particularly when the eyes are involved.
Systemic Immunosuppressive Therapy
The cornerstone of treatment involves systemic immunosuppressive therapy, which targets the aberrant immune response throughout the body. This approach uses medications delivered orally or intravenously to modulate immune system activity and prevent further tissue damage. The goal is to reduce the production of autoantibodies and suppress the inflammatory processes driving disease progression.
Various immunosuppressive medications may be employed, either alone or in combination, depending on disease severity and individual patient factors. These powerful medications work by dampening the overactive immune response that causes tissue damage. While highly effective, immunosuppressive drugs require careful monitoring due to potential side effects and the need to balance disease control against treatment-related risks.
The Importance of Aggressive Treatment
When the eyes are involved, the treatment approach must be particularly aggressive. The substantial risk of vision loss makes ocular involvement a clear indication for intensive immunosuppressive therapy. Without such treatment, the disease progresses in approximately three-quarters of patients, leading to worsening scarring and increasing risk of blindness.
With appropriate immunosuppressive treatment, many patients can achieve remission of their ocular disease. Remission represents a state where disease activity is controlled and progression is halted, though this does not necessarily mean the condition is cured. Maintaining remission requires ongoing treatment and vigilant monitoring to detect any signs of disease reactivation early, when intervention can be most effective.
Addressing Local Ocular Complications
Beyond systemic therapy, treatment must also address the various local complications affecting the eye. Eyelid abnormalities require specific interventions to prevent ongoing trauma to the ocular surface. Misdirected eyelashes may need removal or repositioning to eliminate their damaging effects on the cornea. In some cases, surgical procedures may be necessary to correct eyelid malposition or release adhesions between the eyelid and eyeball.
Ocular surface disease and corneal complications require targeted management strategies. Topical medications help reduce inflammation and promote healing of damaged tissues. Therapeutic contact lenses may be used to protect the cornea and provide a smooth optical surface for improved vision. Treatment of dry eye, a common complication of this condition, involves artificial tears, anti-inflammatory medications, and other supportive measures.
Long-Term Management and Monitoring
Successfully managing this autoimmune eye condition requires a long-term commitment to treatment and regular monitoring. Even after achieving remission, patients need ongoing surveillance to detect disease reactivation early. Regular follow-up appointments allow healthcare providers to assess treatment effectiveness, monitor for complications, and adjust therapeutic strategies as needed.
The Role of Multidisciplinary Care
Optimal management often involves coordination among multiple specialists. Ophthalmologists with expertise in ocular surface disease and autoimmune conditions play a central role in managing the eye manifestations. Rheumatologists or immunologists may be involved in overseeing systemic immunosuppressive therapy. When other body systems are affected, additional specialists contribute to the comprehensive care team.